Have you been diagnosed with gout?
Gout attacks, while intensely painful, fortunately, have a somewhat predictable duration and frequency, although these can vary significantly from person to person. Gout is more than a mere inconvenience characterized by sharp pain, swelling, and general discomfort. This all-too-common but often misunderstood condition can significantly impact our joints as we age. Utilizing my experience as a physical therapist, I will guide you through gout fundamentals, offering clarity and practical strategies for navigating its challenges.
In this guide, we will unravel the critical aspects of this condition, from its underlying causes to effective management strategies. Whether you’re seeking a better understanding of gout or practical tips for maintaining joint health, this article will provide valuable insights that empower you to take control of gout to improve your quality of life.
What is Gout?
Gout, often called “crystal arthritis,” is a distinctive form of arthritis that manifests as acute, intense joint pain. While it can strike various joints, it frequently targets the big toe, making each step painful.
Gout occurs when microscopic urate crystals assemble in the joints, particularly at the big toe. As they accumulate, they trigger inflammation, often reported as feeling like sharp needles inside the joint. It results in pain, swelling, and a telltale redness and discomfort.
For those affected by gout, standing or walking often becomes a formidable challenge; even the slightest movement can elicit discomfort.
Gout demands our attention for the immediate pain it inflicts and the potential long-term implications on joint health. By understanding more about this condition, we can better navigate the associated challenges and work towards a proactive approach to joint health.
Causes of Gout
At its core, gout results from the delicate equilibrium of uric acid in the body being disrupted, triggering a cascade of events that lead to discomfort and inflammation.
The cause of gout lies in the body’s struggle to maintain an equilibrium between the production and elimination of uric acid. Uric acid is a natural byproduct of the breakdown of purines, substances found in various foods and within our cells.
Ordinarily, the body efficiently processes and eliminates uric acid, preventing its accumulation to levels that could precipitate gout. However, uric acid levels soar when this delicate balance falters, forming the crystals that cause joint inflammation.
Several factors conspire to upset the equilibrium of uric acid, setting the stage for gout to make its unwelcome entrance.
- Dietary Choices: Foods rich in purines, such as red meat, seafood, and alcohol, can increase uric acid levels.
- Genetic Predisposition: Some individuals are genetically predisposed to struggle with the efficient processing of uric acid, making them more susceptible to gout.
- Medical Conditions: Certain underlying conditions, such as kidney dysfunction or hypertension, can disrupt uric acid regulation. In these instances, gout may be a symptomatic expression of broader health challenges.
Understanding these contributing factors allows us to adopt a more nuanced approach to managing gout. By recognizing the role of diet, genetics, and medical conditions, we can tailor strategies to address the root causes.
Gout Attacks
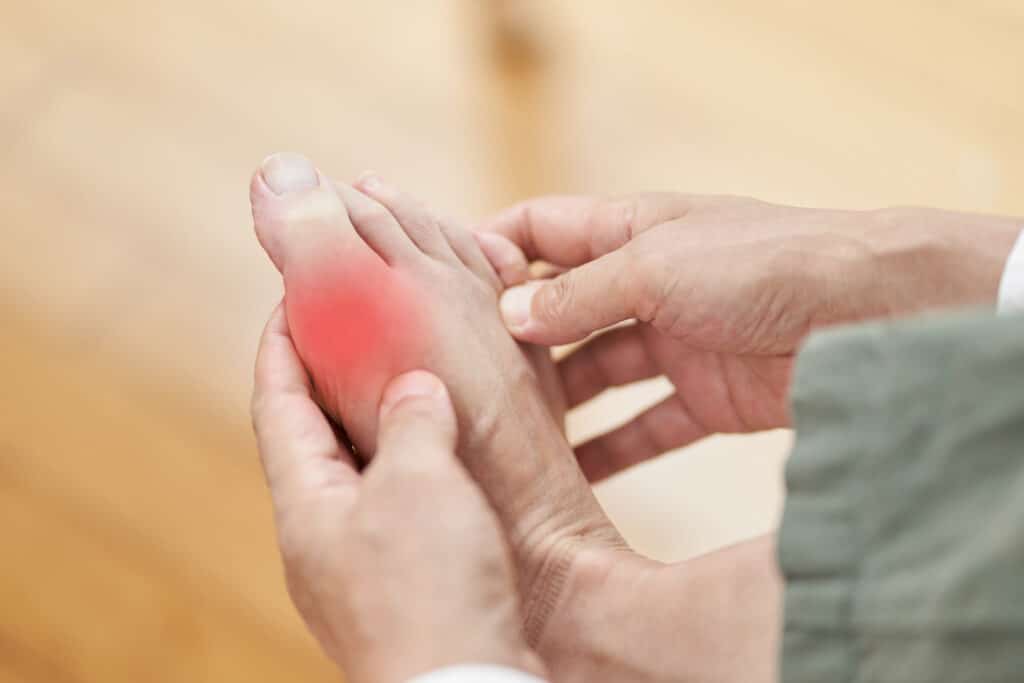
Gout attacks are akin to a sudden, unwelcome lightning storm in your joints, marked by distinct and intense symptoms. This pain is not just a dull ache; it’s a sharp, piercing sensation that can be truly debilitating. The affected joint swells and becomes quite uncomfortable.
The swelling contributes to tenderness, amplifying the pain with contact. Each motion intensifies the discomfort when trying to move that joint, and mobility is often severely compromised.
Coping with Gout Attacks
A plan for enduring a gout attack can make the ordeal more bearable. Here are some of the main approaches that can help you to deal with the discomfort of a gout attack/
Rest: During a gout attack, give your affected joint a break. Minimize movement, avoid putting weight on it, and let it recuperate.
Elevation: Elevating the affected limb can help. Keeping the affected limb above your heart level can facilitate proper circulation and prevent excessive swelling.
Ice: Applying an ice pack to the affected joint helps numb the pain and constrict blood vessels, mitigating inflammation.
NSAIDs: Nonsteroidal anti-inflammatory drugs (NSAIDs) are helpful during a gout attack. Medications like ibuprofen or naproxen can help manage both pain and inflammation.
Rest is your primary strategy for allowing the inflamed joint to heal, but rest doesn’t mean stagnation. Gentle exercises and stretches—also called active recovery—can be useful to keep the joint moving to help lessen the pain from gout attacks.
Slight movements can help you maintain mobility without aggravating the pain. Exercises can be subtle, like flexing and rotating the ankle, or gentle stretches to keep the joint limber. Finding a balance between rest and movement is the key to coping with gout attacks.
How Long Does Gout Last?
Gout attacks, while intensely painful, fortunately, have a somewhat predictable duration and frequency, although these can vary significantly from person to person.
Duration of Attacks
Typically, a gout attack lasts anywhere from a few days to about a week. The onset of an attack is usually quite sudden, with pain peaking in severity within the first 12 to 24 hours. After this peak, the pain gradually subsides, with the joint returning to normal within a week.
However, the exact duration can be influenced by various factors, including treatment efficacy, the individual’s health status, and adherence to lifestyle modifications.
Frequency of Attacks
The frequency of gout attacks is highly variable and uniquely personal. Some individuals may experience sporadic episodes, occurring infrequently and sometimes with years between attacks.
In contrast, others might find themselves grappling with more frequent episodes, primarily if underlying factors like diet, medication adherence, and lifestyle choices are not optimally managed.
Progression Over Time
Initially, gout attacks may be isolated and infrequent, but they can become more frequent and prolonged without appropriate management.
The intervals between attacks, known as intercritical periods, may shorten if uric acid levels remain uncontrolled. This can eventually lead to a more chronic form of gout, where joint discomfort becomes a persistent issue rather than an episodic one.
Predicting and Preparing for Attacks
While it’s challenging to predict the exact timing of a gout attack, individuals who have experienced previous episodes can often recognize early warning signs, such as mild aching in the joints, enabling them to take preemptive measures.
Effective management, including medication, dietary adjustments, and lifestyle modifications, is crucial in reducing the severity and frequency of attacks.
Importance of Long-Term Management
Understanding the potential progression and variability of gout attacks underscores the importance of long-term management strategies, including regular medical follow-ups, adherence to treatment protocols, and lifestyle adjustments.
These measures can significantly impact the course of the disease, helping to reduce both the frequency and severity of future attacks. Recognizing these patterns and adopting comprehensive management strategies are crucial to mitigating the impact of gout on daily life.
Risk Factors and Lifestyle Modifications
As mentioned previously, some common risk factors for developing gout include your dietary choices, family history, obesity, and other medical conditions. Arming yourself against the risk of gout involves making intelligent lifestyle choices that set the stage for a joint-friendly environment.
Some standard advice I will often give my patients includes maintaining a good diet, exercising regularly, and hydrating properly.
Choose a balanced diet incorporating whole grains, fruits, vegetables, and low-fat dairy. Limit the intake of foods high in purines to reduce the risk of gout.
Engage in regular physical activity to help maintain a healthy weight and regulate uric acid levels. Exercise contributes to strengthening your joints, creating an environment less favorable for the development of gout.
Sufficient water intake assists in eliminating excess uric acid from the body, minimizing the chances of crystals forming in your joints.
By recognizing and addressing these risk factors, you develop a proactive approach that empowers you to take charge of your joint health.
How Gout is Diagnosed
Diagnosing gout is not a one-size-fits-all process. The foundation of understanding gout lies in your medical history. It’s more than a mere record of past health issues; it’s a narrative providing context to your joint health story.
Details about your diet, lifestyle, and previous experiences of joint pain contribute to the overall gout narrative.
Once they have a better idea about potential causes, your healthcare provider will conduct a thorough physical examination, concentrating on the affected joint.
In certain instances, a deeper investigation is warranted. Joint fluid analysis might require extracting a sample from the affected joint. This fluid undergoes tests for urate crystals, the definitive evidence of gout. It serves as the confirmation needed for an accurate diagnosis.1
The collaboration of these components—your medical history, physical examination, and joint fluid analysis—enables healthcare professionals to construct a thorough understanding of your joint health.
Treatment Options
Alongside lifestyle modifications, certain drugs can help to speed up the gout recovery process. Your doctor may suggest the following medications.2
Colchicine
Colchicine is a medication designed for fast action during gout attacks. Its primary function is to reduce inflammation, offering rapid relief in the acute phases of gout. It serves as an initial intervention to alleviate joint discomfort.
Allopurinol
Allopurinol takes a more strategic and long-term approach to managing gout. This medication inhibits its production by targeting the root cause—elevated uric acid levels. Acting as a stabilizing force, allopurinol aims to prevent the recurrence of gout attacks.
Collaborating closely with your healthcare provider is essential when navigating the medication landscape, rather than dealing with gout alone. They can customize the prescription based on your situation, ensuring the chosen medications align with your health goals and lifestyle.
Consistency is crucial for preventing future gout attacks. It involves a commitment to sustained well-being, going beyond short-term interventions. Adhering to the principles of a balanced diet, hydration, and regular exercise is an ongoing process.
Consistent, positive lifestyle choices contribute to a joint-friendly environment, reducing the likelihood of gout resurgence.
Periodic check-ins with your healthcare provider form the foundation of long-term prevention. These appointments allow for the monitoring of uric acid levels, adjustment of medications if necessary, and a proactive response to any emerging challenges.
Living with Gout

Living with gout often requires adjustments to daily life to manage symptoms and maintain overall joint health. The following tips can enhance your quality of life when dealing with gout attacks.
- Footwear Selection: Choose shoes that provide ample support and cushioning. Properly supportive footwear helps distribute weight evenly, reducing the strain on affected joints, particularly in the feet, an area most commonly impacted by gout. Look for shoes with a comfortable fit, good arch support, and soft insoles.
- Low-Impact Exercise: Engage in low-impact activities such as swimming, cycling, and gentle stretches. These exercises maintain joint mobility and flexibility while minimizing stress on the joints. Swimming, for instance, is particularly beneficial as the buoyancy of water supports body weight, relieving pressure on the joints.
- Dietary Adjustments: Monitor and limit consumption of purine-rich foods like red meat, seafood, and alcohol, as purines can increase uric acid levels, exacerbating gout symptoms. An anti-inflammatory diet rich in fruits, vegetables, whole grains, and lean proteins can help reduce inflammation and the frequency of gout attacks.
- Hydration: Integrate consistent hydration into your daily routine. Drinking plenty of water helps the body flush out uric acid, the buildup of which causes gout flare-ups. Carrying a water bottle or using a hydration app can be a practical way to ensure you drink enough water throughout the day.
- Heat and Cold Therapy: Use heating pads or cold packs to manage joint discomfort. Heat can relax muscles and increase blood flow, reducing joint stiffness. Conversely, cold therapy can reduce swelling and numb pain. Use cold packs and heating pads for general stiffness during acute flare-ups.
By incorporating these strategies, individuals with gout can better manage their symptoms and maintain an active lifestyle in spite of gout discomfort.
Key Takeaways
- Gout, a form of “crystal arthritis,” primarily affects the big toe and is caused by the build-up of urate crystals, leading to severe joint pain and swelling.
- The condition is triggered by an imbalance in uric acid levels, influenced by dietary habits, genetics, and certain health issues like kidney problems or hypertension.
- Gout attacks present as sudden, intense joint pain and swelling, varying in duration and frequency among individuals.
- Effective management of gout attacks involves rest, elevation, ice application, NSAIDs, and gentle joint exercises.
- Risk factors include diet, genetic predisposition, obesity, and other health conditions, with prevention focused on a balanced diet, exercise, and hydration.
- Diagnosis combines medical history, physical examination, and joint fluid analysis for urate crystals.
- Treatment includes medications like Colchicine for immediate relief and Allopurinol for long-term uric acid level management.
- Long-term prevention requires lifestyle adjustments, medication adherence, and regular medical check-ups.
- Daily management of gout includes supportive footwear, low-impact exercises, dietary monitoring, and hydration.
References
- Tausche, A. K., Jansen, T. L., Schröder, H. E., Bornstein, S. R., Aringer, M., & Müller-Ladner, U. (2009). Gout—current diagnosis and treatment. Deutsches Ärzteblatt International, 106(34-35), 549.
- Wilson, L., & Saseen, J. J. (2016). Gouty arthritis: a review of acute management and prevention. Pharmacotherapy: The Journal of Human Pharmacology and Drug Therapy, 36(8), 906-922.






