Up to 80% of individuals will suffer from back pain at some point in their lives, and in many cases, disc herniation is to blame. Despite being incredibly painful for some people, most cases improve with a few weeks to months of conservative treatment including traditional medicinal and complementary options.
Spinal Anatomy
To better understand what a disc herniation is, let’s briefly discuss the anatomy of the spine.
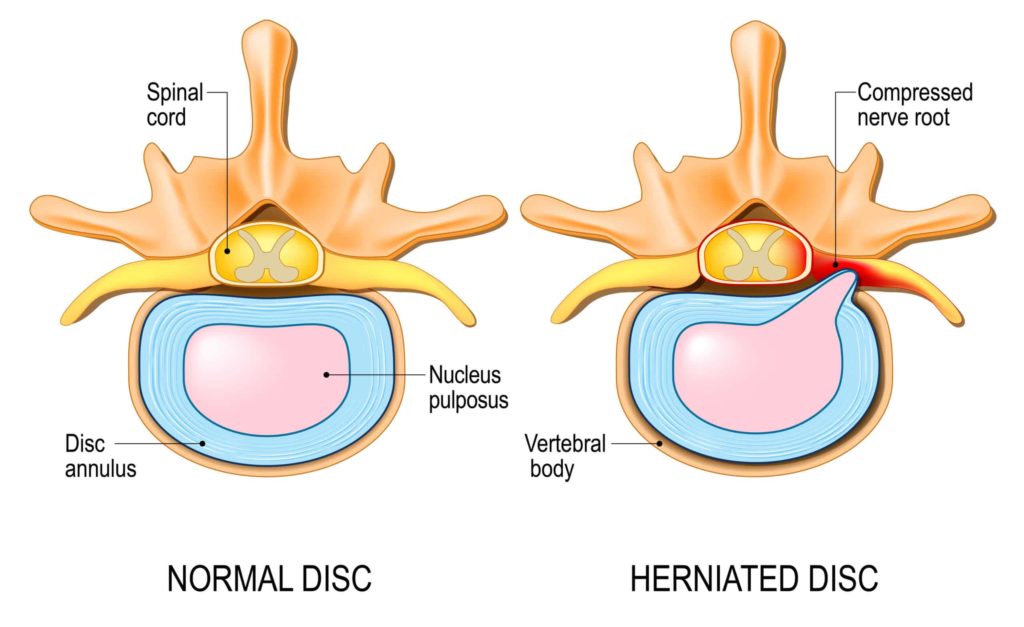
The spine is composed of 24 individual vertebrae that connect to each other via flexible facet joints. An intervertebral disc lies in between each of the spinal vertebrae. Each intervertebral disc is comprised of two layers – the nucleus pulposus, which is the inner, jelly-like, layer, and the annulus fibrosis, which is the outer, fibrous, layer. Not only do the intervertebral discs help to stabilize the spine, they also act as shock absorbers.
What is a Disc Herniation?

A disc herniation happens when the inner, jelly-like, layer ruptures through a weakened spot in the outer, fibrous, layer. A herniated disc can cause inflammation and irritation of surrounding spinal nerves, leading to symptoms including back pain, weakness, and/or numbness in the lower or upper extremities. While disc herniation can occur anywhere in the spine, they most commonly occur in the lower back (lumbar spine) and neck (cervical spine).
Symptoms of Disc Herniation
Symptoms of disc herniation vary widely, with some patients having no symptoms and others having debilitating symptoms, including:
- Pain
- If the disc herniation is in the lower back, pain will likely be experienced in the lower back, buttocks, thigh, calf, and sometimes the foot on the affected side.
- If the disc herniation is in the neck, pain will likely be experienced in the neck, shoulder, and arm on the affected side.
- Pain may intensify with coughing, sneezing, and with certain movements (extension, lateral bending, and/or rotation).
- Numbness or tingling in area that is supplied by the affected nerve.
- Weakness of the muscles supplied by the affected nerve.
Causes of Disc Herniation
Disc herniations are most commonly caused due to wear and tear on the discs; this is known as disc degeneration. Normal aging causes the intervertebral discs to lose a portion of their water content making them more susceptible to injury.
In many cases no underlying cause can be identified; however, improper and/or heavy lifting may cause a disc to herniate, and in rare cases trauma from a slip and fall or car accident may be responsible.
Various risk factors have been identified that increase the risk of disc herniation, including:
- Physically demanding occupations that involve heavy and/or repetitive lifting, pushing, pulling and/or twisting.
- Excess weight placing excess stress on the intervertebral discs.
- Having a genetic predisposition.
Diagnosis of Disc Herniation
In many cases, disc herniation can be diagnosed based on a thorough history and physical examination. The patient history typically includes questions related to the patient’s medical history, their family history, as well as questions specific to their current symptoms. The physical examination typically involves inspection and palpation of the affected area, range of motion testing, neurological testing including reflexes and sensation, muscle testing and orthopedic testing specific to the area involved. Additional testing, such as X-ray, computed tomography (CT), magnetic resonance imaging (MRI), and myelogram may be recommended to confirm disc herniation diagnosis and rule out other pathology that may be causing symptoms. In order to determine if there is associated nerve damage, and to determine the location and extent of damage, nerve conduction studies may also be recommended.
Treatment for Disc Herniation
First line disc herniation treatment typically includes pain and anti-inflammatory medication, as well as muscle relaxants. Short term narcotic therapy, and antidepressants, may be recommended in cases that don’t respond to first-line medication options. In persistent cases, epidural steroid injections or nerve blocks, may be recommended.
In addition to traditional medicinal therapy, a trial of physical therapy or chiropractic may be recommended. Treatment may include the use of various modalities include ice and heat therapy, electrical stimulation, ultrasound, traction, and/or manual therapy. Patients will also be educated on proper lifting techniques and be provided with an exercise program to increase range of motion and strength in the affected area.
In cases that do not respond to conservative therapy, surgery may be necessary. Various surgical options exist depending on the location and extent of the disc herniation.
Conclusion
Back pain is a common condition experienced by millions of people, and disc herniation is often the culprit. Disc herniation can cause an array of symptoms including pain, numbness, tingling, and/or weakness. Treatment for disc herniation often involves a combination of therapies including traditional medicinal options and alternative treatment options. However, in some cases, surgery may be necessary. Patients suffering with symptoms of disc herniation are encouraged to speak to their physician to determine what treatment options are best for their condition.
Sources
https://www.mayoclinic.org/diseases-conditions/herniated-disk/symptoms-causes/syc-20354095
https://orthoinfo.aaos.org/en/diseases–conditions/herniated-disk-in-the-lower-back/
https://www.ncbi.nlm.nih.gov/books/NBK279472/
https://www.aans.org/Patients/Neurosurgical-Conditions-and-Treatments/Herniated-Disc